How Diabetes Affects the Eyes
Diabetes is a disease that affects the body's ability to process and store sugar. Over time, chronically high blood sugar levels severely damage the tiny, delicate blood vessels throughout the body—including the micro-vessels inside the retina (the light-sensitive tissue at the back of the eye).
This damage is called Diabetic Retinopathy, and it is a leading cause of blindness in adults.
Why Does My Vision Fluctuate?
Before retinopathy even occurs, patients often experience wild swings in their prescription. When blood sugar spikes, the crystalline lens inside your eye literally swells with fluid, causing sudden, extreme nearsightedness. When blood sugar drops, the lens deflates. If your vision changes from day to day, it is a major warning sign of uncontrolled blood sugar.
Signs & Symptoms
Early stages often have NO symptoms.- Blurred or Patchy Vision: Central vision may become blurry or have missing “blank” spots.
- Sudden Floaters: A sudden shower of dark spots or “cobwebs” can indicate a bleeding vessel in the eye.
- Color Washed Out: Colors may appear faded or desaturated.
- Poor Night Vision: Difficulty seeing in low light or while driving at night.
Type I vs. Type II Diabetes
The screening guidelines for diabetic retinopathy depend heavily on the type of diabetes you have, as the onset of the disease behaves differently.
Type 1 Diabetes
Rapid OnsetBecause Type 1 is an autoimmune condition that usually presents suddenly with severe symptoms, doctors know exactly when the disease started.
Type 2 Diabetes
Gradual OnsetType 2 diabetes can develop silently over many years. By the time a patient is officially diagnosed by their physician, they may have had elevated blood sugar for a decade.
The Stages of Diabetic Retinopathy
Mild Non-Proliferative (NPDR)
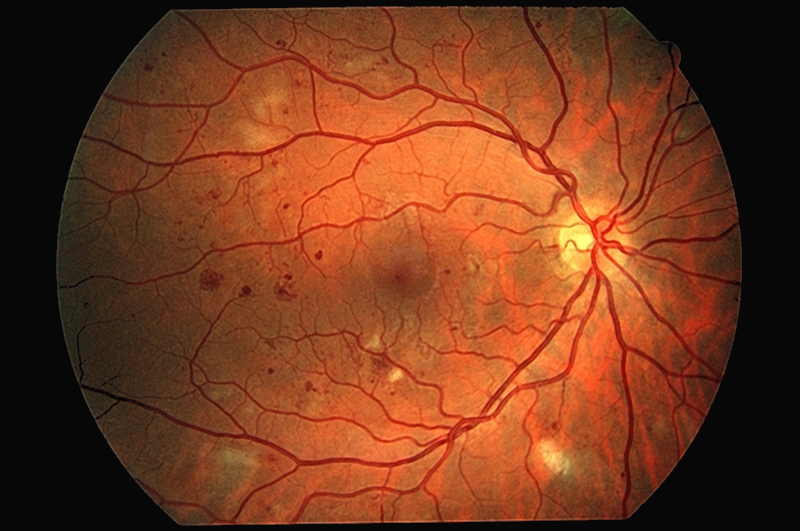
The earliest stage. Microscopic balloon-like swelling occurs in the retina's tiny blood vessels (microaneurysms). These may leak small amounts of blood or fluid into the retina.
Moderate to Severe NPDR
As the disease progresses, blood vessels that nourish the retina become blocked. The retina becomes starved of oxygen (ischemia), leading to larger hemorrhages and “cotton wool spots” (areas of dead nerve tissue).
Proliferative Diabetic Retinopathy (PDR)
The most advanced and dangerous stage. The oxygen-starved retina sends signals to grow new, abnormal blood vessels (neovascularization). These fragile vessels easily break, leaking blood into the center of the eye (vitreous hemorrhage). The resulting scar tissue can contract and cause a Tractional Retinal Detachment, leading to permanent blindness.
Diabetic Macular Edema (DME)
At any of the stages above, fluid can leak into the macula (the center of the retina responsible for sharp, straight-ahead vision). This swelling causes severe blurry vision and is the most common cause of vision loss in diabetic patients.
A Collaborative Medical Approach
Managing diabetes requires a team. Dr. Fouladian acts as your ocular diagnostic hub.
Dr. Fouladian (Optometry)
Performs your mandatory annual Dilated Exam or Optomap® Retinal Imaging to look for the earliest signs of bleeding or swelling. We monitor your eyes closely to catch changes before vision loss occurs.
Primary Care Physician (PCP)
Systemic control is the only way to stop the disease. After your eye exam, Dr. Fouladian sends a detailed medical report directly to your PCP or Endocrinologist to help them adjust your A1C, blood pressure, and cholesterol medications.
Retina Specialist
If your disease progresses to severe NPDR, PDR, or Macular Edema, Dr. Fouladian fast-tracks your referral to elite Retina Specialists in Los Angeles. They provide sight-saving treatments like Anti-VEGF injections or Laser Photocoagulation to stop the bleeding.
Don't Wait for Symptoms
If you have diabetes, an annual dilated eye exam is medically mandatory. Medicare and most medical insurances cover this essential preventative care.
